The world of healthcare is rapidly innovating to meet the needs of a growing and ageing Australian population. As clinicians are faced with treating increasingly complex and multifaceted health conditions, the burden on our healthcare systems grows and there is a need to ‘do more with less’.
Artificial Intelligence (AI) presents exciting opportunities in the world of medicine to meet these challenges. From machine learning revolutionising the way we analyse data, to robotics providing surgeons with increased control and precision in their work, we explore how AI is changing the face of healthcare.
What is AI in Medicine?
The traditional evidence based approach to medicine uses statistical methods where mathematical equations characterise patterns within data. AI utilises ‘machine learning’ (ML) to determine more intricate and complex links in data. ML will weigh up evidence to reach reasoned verdicts, just the way a clinician does.
The key to AI is that the reasoning is done exponentially faster, taking into account more data – often more accurately than what a clinician may be able to. For example, the NHS in North London is successfully trialling a smartphone app to triage 1.2 million people instead of having them call an overburdened emergency line.
The most important factor about AI in medicine is the ability to rapidly learn from each individual case that is assessed, meaning that AI can constantly add to its dataset. This approach means AI can gain more knowledge from more cases than a single clinician could in their whole career.
How is AI currently being used in medicine?
AI is currently being used in medicine in a range of different ways.
Diagnosis and Management
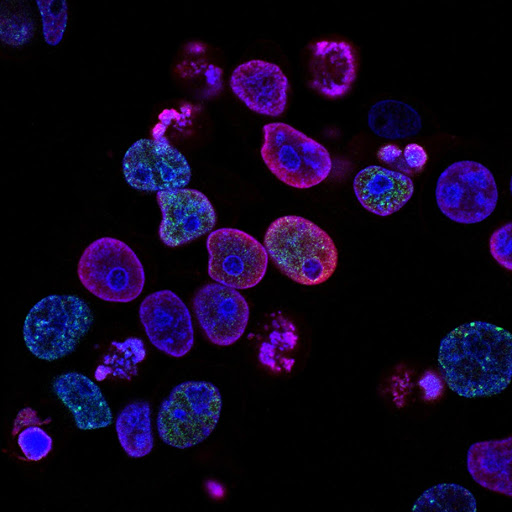
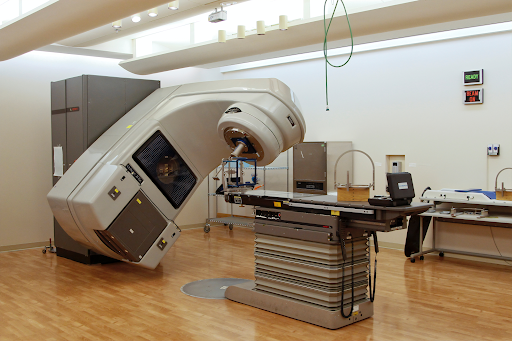
One of the ways AI is rapidly advancing medicine is in image detection. Currently dermatologists are being outperformed by AI-driven applications when it comes to correctly identifying benign or malignant skin lesions. Additionally, AI is being used to identify more accurate and specific target regions for head and neck radiotherapy as well as identifying pulmonary tuberculosis on chest radiographs.
AI systems are also being developed to interpret other image data such as radiographs, ultrasounds and retinal scans. These fall under the banner of what’s called Deep Learning, where AI will use previous image data sets to learn adaptively about benign and malignant lesions. This information will be matched with patient history and genomic information to “see” beyond what the human eye could for early detection of cancerous lesions.
Precision Medicine
Precision medicine is an emerging medical field which incorporates AI to proactively treat disease. It is concerned with preventing just as much as reacting to disease and disorder. AI will utilise genomic information to make diagnosis and treatment recommendations for some cancers. There exists huge variation in genetic profiles that can be complex for doctors and specialists to understand when it comes to predicting risk for patients.
Supporting Medical Staff and Poorly Resourced Services
For many hospitals, it’s administrative tasks that take up a huge majority of time for staff. AI promises to reduce some of this load. In speech recognition and language processing, AI can transcribe patient interactions, analyse clinical notes and prepare records such as radiology reports for doctors. The clinician naturally checks over, and where necessary, amends the generated paperwork, but they still save considerable time.

AI can also support large, underserviced populations. A recent study in Deep learning demonstrated that AI could accurately classify TB via chest radiographic images with a sensitivity of 97.3% and a specificity of 100%. Imagine a country with a high prevalence of TB and an under-serviced medical system or areas with a lack of radiology equipment, operators or clinicians. A single AI-driven system could make all the different in the diagnosis and subsequent speedy management of TB-infected patients.
What is the future of AI in healthcare?
The future of AI in medicine is bright.
Precision Medicine: Diagnosis, Treatment, and Management
In the same way that AI will interpret data from medical trials, it can learn from and interpret a vast array of patient information, from history, to genomic information, to lifestyle. AI can take a patient’s information and create tailored management plans for that patient, as opposed to the historic ‘one-size-fits-all’ approach that medicine currently uses. Using the enormous amount of information at hand, AI can predict which management protocols will most likely lead to results based on the patient’s specific information.
Additionally, AI can predict both an individual’s and a particular population’s risk of a certain disease or disorder, from cancer to more complex disease like diabetes and chronic heart failure. As we see more in-home devices being used, AI can begin to take into account information beyond historical and physiological. It may be able to predict disease based on lifestyle factors, environment and socio-economic information.
Preventative Medicine
A huge upcoming field for AI will be in the prevention of disease. As mentioned above, AI can learn, based on data, what the risk of disease may be in an individual population. This will only improve as AI is used more and the data set increases.
Additionally, AI will begin to play a role in helping patients in their compliance with recommendations to prevent disease. If we consider that health advice is only helpful if individuals take it on, we realise that many preventable diseases can be avoided if an individual is given the right kind of advice. This is where AI will come in. It can base advice on real world examples and tailor health advice to individuals.
This ‘nudge’ technology is already in place. Think about your smartphone running app notifying you that you haven’t run in two weeks. AI will not only begin to utilise smartphones, smart watches and other devices to nudge you in the right direction, but will also predict what kinds of recommendations you will most likely follow in order to achieve the health status you require to prevent a certain disease.
Will AI Replace Doctors?

This is a common fear. The simple answer is no. Machines have no capacity for empathy or compassion. As a result, AI will ultimately be used to support clinicians and not to replace them.
In our example above, while AI was used to identify zones for radiotherapy, a clinician was still the one who administered the therapy. In surgical suites, the surgeon makes all decisions. Surgical robots just increase the surgeon’s visibility and allow them to make more precise and less invasive incisions.
There are also medical ethics to consider, alongside data privacy and collection. For now though, the future of AI is exciting as it potentially promises us a healthier future.
References
- Esteva A, Kuprel B, Novoa RA, et al. Dermatologist-level classification of skin cancer with deep neural networks. Nature. 2017;542(7639):115–118.
- Buch VH, Ahmed I, Maruthappu M. Artificial intelligence in medicine: current trends and future possibilities. Br J Gen Pract. 2018;68(668):143‐144. doi:10.3399/bjgp18X695213
- Lakhani P, Sundaram B. Deep learning at chest radiography: automated classification of pulmonary tuberculosis by using convolutional neural networks. Radiology. 2017;284(2):574–582.
- Davenport T, Kalakota R. The potential for artificial intelligence in healthcare. Future Healthc J. 2019;6(2):94‐98. doi:10.7861/futurehosp.6-2-94